Twenty years ago this September, 80 organizations representing healthcare professionals and consumers nationwide joined the American Chronic Pain Association to establish “Pain Awareness Month.” The intent of the annual observation—to improve recognition, understanding, and treatment of severe pain—is perhaps even more relevant now than it was at its founding. Today, a staggering 100 million Americans suffer from significant pain and its ill effects.
Many among that group have advanced-stage cancer. And according to the National Cancer Institute, 80% of cancer patients have moderate to severe pain that negatively affects their functional status and quality of life. Beyond the symptoms of cancer itself, treatment for the disease—including radiation, chemotherapy, and other drugs—may produce unwanted side effects, resulting in painful or uncomfortable new issues such as swelling, nausea, shortness of breath, even depression.
But regardless of the cause, you don’t have to live with chronic, serious pain. Through sophisticated technology and precision pain relief, Capital Caring Health’s Schaufeld Family Advanced Pain Clinic (SAPC) can help you or your loved one return to the comforts of simple daily activities and to the pursuits that bring joy.
Advanced Treatment for Advanced Pain
Patients are typically referred to SAPC when pain becomes severe, and medication, the most common treatment, is no longer effective. While the majority of SAPC’s patients have cancer, the clinic can also help with the symptoms and side-effects of dementia, congestive heart failure, chronic obstructive pulmonary disease, osteoarthritis, neuropathy, and neurological diseases (Multiple Sclerosis, Parkinson’s Disease, ALS).
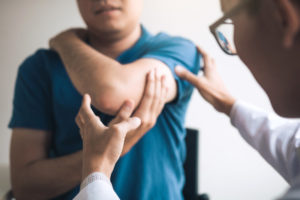
The process begins with evaluating the patient for limitations, mobility problems, and other major issues that may affect treatment options and outcomes. Then the team uses the most advanced technology and imaging techniques to arrive at the correct diagnosis and a minimally invasive intervention plan that targets pain at the source.
“We start with the most effective, conservative approaches, and expand to sophisticated, surgical interventions as needed to bring relief from pain and discomfort,” says Michael Byas-Smith, MD, Medical Director of the clinic, and a well-known expert in pain management with decades of experience with cancer patients. “The techniques we perform are better and safer than the long-term use of general oral or intravenous analgesic/pain relievers and opioids, which carry their own set of problems.”
The expertise of Dr. Byas-Smith and the clinic in the successful use of interventional pain relief is well-known throughout the mid-Atlantic region and has attracted referrals from some of the region’s most prominent health systems. As a result, the SAPC frequently treats patients from INOVA’s Schar Cancer Institute at Fairfax Hospital, Johns Hopkins Kimmel Cancer Center at Sibley Memorial Hospital, Medstar Georgetown Lombardi Comprehensive Cancer Center, and others.
In every case, Dr. Byas-Smith works with the patient’s oncologist, neurologist, internist, or other referring physician so they know the details of the diagnosis and treatment. Some pain interventions may affect or interact with other therapies prescribed for the underlying disease.
At the Forefront of Pain Management
Capital Caring Health’s Schaufeld Family Advanced Pain Clinic offers a full range of pain intervention, including:
- Neurolytic therapies to block pain for extended periods of time often resulting in increased mobility, reduced or elimination of opioid (morphine) medications and often complete relief of pain.
- Intrathecal pump therapies, whereby an implanted pump delivers medication directly to the spinal cord.
- Epidural and major joint injections to reduce pain and improve mobility.
- Injections for axial spine fractures.
- Aspiration (paracentesis or thoracentesis) to remove excess fluid from the abdomen or lungs, respectively, reducing discomfort and improving breathing.
In fact, as a single provider, Dr. Byas-Smith performs more abdomen and lung aspirations than any other group in the region. This service eliminates many ER visits and hospitalizations for our clients. CCH treats patients right in the clinic for expedited care and patient convenience. Dr. Byas-Smith is also a proponent of withdrawing all of the excess fluid, versus the partial extraction most providers do nowadays.
“Removing all of the accumulated fluid provides a greater benefit to the patient,” says Dr. Byas-Smith, who is gathering data on the effectiveness of total removal for analysis and publication. “Performing the aspiration right in the clinic is also much more cost effective than expensive emergency room or hospital care. I hope my experience and success with total aspiration may influence the traditional practice industry-wide for better patient outcomes and greater cost efficiency.”
Care for the Whole Person
Even when they share the same diagnosis with others, each patient who seeks care for severe pain is completely different. Such factors as stage of illness, pain tolerance, coping abilities, family dynamics, and more can all influence how a patient experiences pain. However, the condition is always most effectively managed by caring for the whole person, and not just treating the symptom.
At CCH, additional services may also help someone cope with pain by treating depression, emotional, and spiritual distress. We offer many types of counseling and support groups for individuals and families.
The pain clinic began as a place to treat the advanced symptoms of CCH hospice patients and has grown to help other patients in our care, as well as the broader community. Building on our reputation—with the generous support of the Schaufeld family—we are poised to do more.
But relieving pain and suffering will always be at the heart of our program.
Says Dr. Byas-Smith, “Patients come in with pain, and we help them leave to have a better day, and a better quality of life.”
To learn more, please call the Capital Caring Health helpline 24/7 at (800) 869-2136.

 Kathleen Ramkaran, RN, CCM
Kathleen Ramkaran, RN, CCM Hali Gantumur
Hali Gantumur Yasmin
Yasmin  Jennifer Olsen GNP-BC
Jennifer Olsen GNP-BC Dr. Cheryl-Lynne McCalla, DO
Dr. Cheryl-Lynne McCalla, DO Meena Raj, MD,
Meena Raj, MD,  Catherine McGrady, RN, MSN, is Vice President, Clinical Programs at Capital Caring Health. In this role she is responsible for the development, implementation, and monitoring of clinical programs in support of high-quality patient-centered care delivery across the continuum of services. Catherine also manages external partnerships including Capital Caring Health’s participation in ACOs and other value-based clinical programs
Catherine McGrady, RN, MSN, is Vice President, Clinical Programs at Capital Caring Health. In this role she is responsible for the development, implementation, and monitoring of clinical programs in support of high-quality patient-centered care delivery across the continuum of services. Catherine also manages external partnerships including Capital Caring Health’s participation in ACOs and other value-based clinical programs Catherine Kravolec
Catherine Kravolec Sherri Parker
Sherri Parker Anne Young
Anne Young Odessa Simpson
Odessa Simpson Hope Collazo
Hope Collazo LaWanda Middleton
LaWanda Middleton Sally Hughes
Sally Hughes Jennifer Godwin
Jennifer Godwin Henry Fuller
Henry Fuller Margaret Doherty
Margaret Doherty Evan Kirschner
Evan Kirschner Gabby True
Gabby True Carla Thompson
Carla Thompson Shannon Collier
Shannon Collier Annette Lindsay
Annette Lindsay Jason Sobel, MD
Jason Sobel, MD Brenan Nierman
Brenan Nierman Susan Roberts
Susan Roberts Jackie Gouline
Jackie Gouline Stacy Brown
Stacy Brown Kremena Bikov
Kremena Bikov


 Audrey Easaw
Audrey Easaw
 Julia Feldman
Julia Feldman Gus has been a part of the Capital Caring Health family for nearly fifteen years. Ten of those years have been in leadership, working with colleagues and co-workers to achieve the best in their ability while promoting CCH core values. Gus has a background in nursing and a lifelong passion for technology. In each position at CCH, Gus has found ways to integrate technology to enhance outcomes and job satisfaction.
Gus has been a part of the Capital Caring Health family for nearly fifteen years. Ten of those years have been in leadership, working with colleagues and co-workers to achieve the best in their ability while promoting CCH core values. Gus has a background in nursing and a lifelong passion for technology. In each position at CCH, Gus has found ways to integrate technology to enhance outcomes and job satisfaction. Pat Bishop
Pat Bishop Elizabeth Ariemma
Elizabeth Ariemma Joe Murray
Joe Murray

 Lin Maurano
Lin Maurano Dwayne Barton, NP
Dwayne Barton, NP Jacob Phillips, MD
Jacob Phillips, MD Tabitha Gingerich, NP
Tabitha Gingerich, NP Donna Smith
Donna Smith Paulette Davidson, Chaplain
Paulette Davidson, Chaplain Colleen Carberry, RN Case Manager
Colleen Carberry, RN Case Manager Sherri Parker, Team Leader Medical Social Worker
Sherri Parker, Team Leader Medical Social Worker Steven Skobel’s Story
Steven Skobel’s Story Marrygold Ugorji’s Story
Marrygold Ugorji’s Story Sulaiman Bangura’s Story
Sulaiman Bangura’s Story Neil Parker’s Story
Neil Parker’s Story Michael Toohig’s Story
Michael Toohig’s Story Liberating Europe
Liberating Europe Hershell Foster
Hershell Foster Hank Willner, M.D.
Hank Willner, M.D. Laura Branker
Laura Branker Jason Parsons
Jason Parsons Altonia Garrett
Altonia Garrett
 Kieran Shah
Kieran Shah Mandy Brouillard
Mandy Brouillard
 Sherri Parker
Sherri Parker Sayaka Hanada
Sayaka Hanada Caitlin Geary
Caitlin Geary Heidi Young
Heidi Young Linda Biedrzycki
Linda Biedrzycki Heidi Young, M.D.
Heidi Young, M.D. Jason Sobel, M.D.
Jason Sobel, M.D. Anne Silao-Solomon, M.D.
Anne Silao-Solomon, M.D.

 Mohammad Saleem, M.D.
Mohammad Saleem, M.D. Maleeha Ruhi, M.D.
Maleeha Ruhi, M.D. Christopher Pile, M.D.
Christopher Pile, M.D. Cameron Muir, M.D.
Cameron Muir, M.D. Fellowship
Fellowship John McCue, D.O.
John McCue, D.O. Peyman Mamdouhi, D.O.
Peyman Mamdouhi, D.O. Adam Knudson, M.D.
Adam Knudson, M.D. Amanda Keerbs, M.D.
Amanda Keerbs, M.D. Matthew Irwin, M.D., M.S.W.
Matthew Irwin, M.D., M.S.W. Alan Goldblatt, M.D.
Alan Goldblatt, M.D. Jennifer Gerhard, D.O.
Jennifer Gerhard, D.O. Ray Jay Garcia, M.D.
Ray Jay Garcia, M.D. Tamara Barnes, M.D.
Tamara Barnes, M.D. Petros
Petros  Shaz Anwar, D.O.
Shaz Anwar, D.O. Lee-Anne West, M.D.
Lee-Anne West, M.D.
 Melissa McClean, N.P.
Melissa McClean, N.P. Michael Byas-Smith, M.D.
Michael Byas-Smith, M.D. Nancy Cook
Nancy Cook Kimberly Grove, CHPO,
Kimberly Grove, CHPO,  Steve Cone
Steve Cone Eric De Jonge, M.D.
Eric De Jonge, M.D. David Schwind
David Schwind Vivian Hsia-Davis
Vivian Hsia-Davis Cameron Muir, M.D.
Cameron Muir, M.D. Keith Everett
Keith Everett Susan Boris
Susan Boris Carolyn Richar
Carolyn Richar
